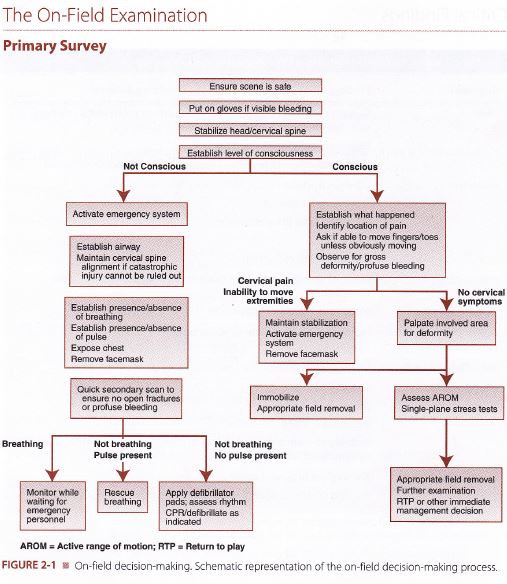
Initial Assessment
Check ABC's.
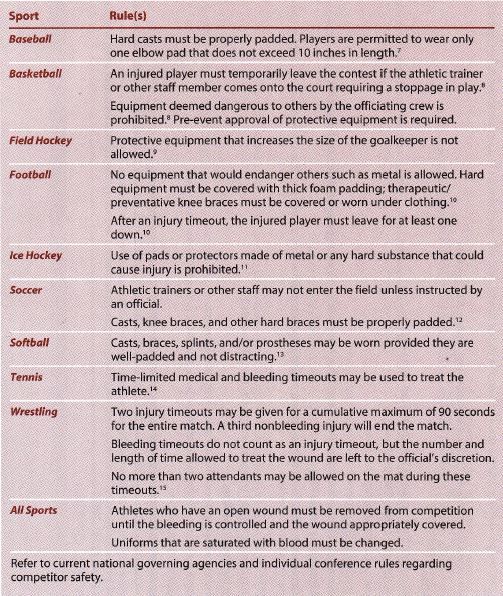
Sports Specific Rules Affecting Examination During Athletic Competition
Secondary Assessment
|
Once the initial assessment is complete, a secondary assessment can begin for the evaluation of an injury.
During a secondary assessment using the Look, Feel, Move process is a great technique to avoid missing anything, as well as ensuring a thorough evaluation. The examiner will first inspect and look at the injured area, next the examiner will feel and palpate, and lastly the examiner will have the athlete move in order to assess ROM, muscular strength, and perform special tests all to come to a clinical impression of the athlete’s injury. Parts of a Secondary Assessment Obtain history:
Observation:
Palpation:
Movement:
Plan:
-Physician referrals |
Retrieved on November 9, 2014 from http://www.youtube.com/watch?v=g8xtOqZFTwo.
Injury Evaluation Form
When doing an injury evaluation it is a good idea to take notes to ensure that you go through each section of an evaluation. A SOAP note form or injury report form are two of the most common types of evaluation protocols used in by healthcare providers today.
SOAP Note
Subjective
This section includes everything that the athlete is telling the health care provider about the injury.
How they did it, when they did it, how bad it hurts, and any other details about the injury and themselves that pertain to the injury (sport, position, previous injuries, etc.).
Objective
This section will contain anything that the healthcare provider finds.
Swelling, discoloration, point tenderness, positive test findings, ROM, MMT, etc.
Action
This section will contain what was done for the injury that day.
Rehab, modalities, etc.
Plan
This section will contain the plan of action for the injury and the athlete’s RTP.
Rehab plan, doctor’s visits, schedule other appointments/tests, etc.
INJURY REPORT FORM
There are many variations of an injury evaluation report, and each individual may have their own depending on where they work. This is a common format of a report form that follows the SOAP note procedures but goes a little more in depth.
Reason for visit:
This section will contain questions for the athlete about why they came in to be evaluated
Chief complaint: What is the main reason that the athlete came in today?
Ex. Right Shoulder pain
Side complaint: Is the chief complaint causing any other problems?
Ex. Athlete is unable to put on a jacket or pick up their backpack due to right shoulder pain.
Subjective:
This section will contain questions for the athlete about what they are feeling, what they did, and will allow the athlete to explain everything to the healthcare provider before they start the evaluation.
Previous History:
Have they ever hurt this shoulder in the past?
Ex. Athlete had a labral tear in the right shoulder one year ago- surgically repaired
Onset:
Was this a sudden onset or gradual?
MOI:
How did the injury occur?
Pain:
The healthcare provider can have the athlete rate the pain on a scale of 1-10.
Audibles:
Did the athlete hear anything when they hurt themselves? Pop? Crack?
Activities that increase/ decrease pain:
What causes the pain and is there anything that makes it better? Does rest help? Does activity make it worse?
Medications:
Did they take any medicine to try to help the pain? Are they on any other medications for this injury or that could affect the injury?
Other details:
Health care provider is looking for any other details that may be pertinent to the injury. What sport do they play and what position? How long have they played the sport? Has their sleep been affected? Do they have a job, and if so what do they do? Etc.
Objective:
This section will contain questions and tests for the health care provider to evaluate the injury. There are 5 subparts to this section in order to thoroughly evaluate the injury as best as possible.
Visual Inspection:
Swelling:
Is there any swelling in the area of the injury?
Discoloration:
Is there any discoloration in the surrounding area of the injury?
Deformity:
Are there any deformities seen in the surrounding area of the injury?
Other:
Is there anything else visual in the area of the injury that needs to be noted?
Palpation:
Point of Tenderness:
Where is the athlete feeling the most pain during palpation?
Heat:
Is there any heat sensed during the evaluation?
Deformity:
Does the health care provider feel a deformity while palpating the area?
Crepitus:
Is any crepitus felt while doing the palpation?
Other:
Is anything else felt during the palpation that needs to be noted?
Functional Assessment:
This section tests the functional movements of the injury, while being compared bilaterally. For each of the following range of motions, notes should be taken on if the athlete is able to complete the ROM to the same degree as the uninjured side, if they show a lack of ROM or weakness on the injured side, or anything that may seem different when compared bilaterally.
AROM: Active range of motion
PROM: Passive range of motion (health care provider moves the athlete through the ROM)
RROM: Resistive range of motion (health care provider provides resistance throughout the ROM)
Other Functional Assessments:
MMT:
Manual Muscle Testing should be done on the injured side and compared bilaterally to the uninjured side. The 1-5 scale MMT scale should be used to assess muscles of the area. The chart can be found on the top of this page.
Neurological:
Neurological assessment can be done by testing sensation, using a sharp/ dull sensation, or other techniques that can be found on the neurological page of this website.
Special Tests:
In this section of the evaluation, the health care provider will perform special tests (examples and lists can be found under the special test tab on this website) to the injured side and then compared bilaterally to the uninjured side. Positive findings should be expressed in this section.
Clinical Impression:
In this section, the examiner can express what they believe is wrong with the athlete.
Plan:
This section includes the steps in which the health care provider plans to do with the injured athlete. This can include on-site treatment (modalities, rehab, etc.), home treatment plan (rest, ice, NSAIDs, etc.), Physician referrals if needed, and any other details of a plan for the athlete’s injury.
When doing an injury evaluation it is a good idea to take notes to ensure that you go through each section of an evaluation. A SOAP note form or injury report form are two of the most common types of evaluation protocols used in by healthcare providers today.
SOAP Note
Subjective
This section includes everything that the athlete is telling the health care provider about the injury.
How they did it, when they did it, how bad it hurts, and any other details about the injury and themselves that pertain to the injury (sport, position, previous injuries, etc.).
Objective
This section will contain anything that the healthcare provider finds.
Swelling, discoloration, point tenderness, positive test findings, ROM, MMT, etc.
Action
This section will contain what was done for the injury that day.
Rehab, modalities, etc.
Plan
This section will contain the plan of action for the injury and the athlete’s RTP.
Rehab plan, doctor’s visits, schedule other appointments/tests, etc.
INJURY REPORT FORM
There are many variations of an injury evaluation report, and each individual may have their own depending on where they work. This is a common format of a report form that follows the SOAP note procedures but goes a little more in depth.
Reason for visit:
This section will contain questions for the athlete about why they came in to be evaluated
Chief complaint: What is the main reason that the athlete came in today?
Ex. Right Shoulder pain
Side complaint: Is the chief complaint causing any other problems?
Ex. Athlete is unable to put on a jacket or pick up their backpack due to right shoulder pain.
Subjective:
This section will contain questions for the athlete about what they are feeling, what they did, and will allow the athlete to explain everything to the healthcare provider before they start the evaluation.
Previous History:
Have they ever hurt this shoulder in the past?
Ex. Athlete had a labral tear in the right shoulder one year ago- surgically repaired
Onset:
Was this a sudden onset or gradual?
MOI:
How did the injury occur?
Pain:
The healthcare provider can have the athlete rate the pain on a scale of 1-10.
Audibles:
Did the athlete hear anything when they hurt themselves? Pop? Crack?
Activities that increase/ decrease pain:
What causes the pain and is there anything that makes it better? Does rest help? Does activity make it worse?
Medications:
Did they take any medicine to try to help the pain? Are they on any other medications for this injury or that could affect the injury?
Other details:
Health care provider is looking for any other details that may be pertinent to the injury. What sport do they play and what position? How long have they played the sport? Has their sleep been affected? Do they have a job, and if so what do they do? Etc.
Objective:
This section will contain questions and tests for the health care provider to evaluate the injury. There are 5 subparts to this section in order to thoroughly evaluate the injury as best as possible.
Visual Inspection:
Swelling:
Is there any swelling in the area of the injury?
Discoloration:
Is there any discoloration in the surrounding area of the injury?
Deformity:
Are there any deformities seen in the surrounding area of the injury?
Other:
Is there anything else visual in the area of the injury that needs to be noted?
Palpation:
Point of Tenderness:
Where is the athlete feeling the most pain during palpation?
Heat:
Is there any heat sensed during the evaluation?
Deformity:
Does the health care provider feel a deformity while palpating the area?
Crepitus:
Is any crepitus felt while doing the palpation?
Other:
Is anything else felt during the palpation that needs to be noted?
Functional Assessment:
This section tests the functional movements of the injury, while being compared bilaterally. For each of the following range of motions, notes should be taken on if the athlete is able to complete the ROM to the same degree as the uninjured side, if they show a lack of ROM or weakness on the injured side, or anything that may seem different when compared bilaterally.
AROM: Active range of motion
PROM: Passive range of motion (health care provider moves the athlete through the ROM)
RROM: Resistive range of motion (health care provider provides resistance throughout the ROM)
Other Functional Assessments:
MMT:
Manual Muscle Testing should be done on the injured side and compared bilaterally to the uninjured side. The 1-5 scale MMT scale should be used to assess muscles of the area. The chart can be found on the top of this page.
Neurological:
Neurological assessment can be done by testing sensation, using a sharp/ dull sensation, or other techniques that can be found on the neurological page of this website.
Special Tests:
In this section of the evaluation, the health care provider will perform special tests (examples and lists can be found under the special test tab on this website) to the injured side and then compared bilaterally to the uninjured side. Positive findings should be expressed in this section.
Clinical Impression:
In this section, the examiner can express what they believe is wrong with the athlete.
Plan:
This section includes the steps in which the health care provider plans to do with the injured athlete. This can include on-site treatment (modalities, rehab, etc.), home treatment plan (rest, ice, NSAIDs, etc.), Physician referrals if needed, and any other details of a plan for the athlete’s injury.